Gensler Healthcare Practice Leader, Tatiana Guimaraes, says updating the design process will enable short and long-term efficiencies.

“Finance drives the world, and we all know that, but we’re dealing with patient care.”
When talking about the challenges affecting healthcare construction these days (labor and supply chain shortages, etc.) Gensler Healthcare Practice Leader, Tatiana Guimaraes, highlights what’s most important.
Building or redeveloping spaces that enable good patient care — today and in the future — as quickly and efficiently as possible.
Which is why Guimaraes advocates for an evolved design process that is more collaborative. Because if everyone involved, (from owners to subcontractors) has a seat at the table from the outset, you can adapt your design plan to address challenges as they arise, she says.
“If we have a contractor on board and they say, ‘Hey, I’m noticing this today,’” then maybe you can change the order of design to address whatever that issue might be, Guimaraes notes.
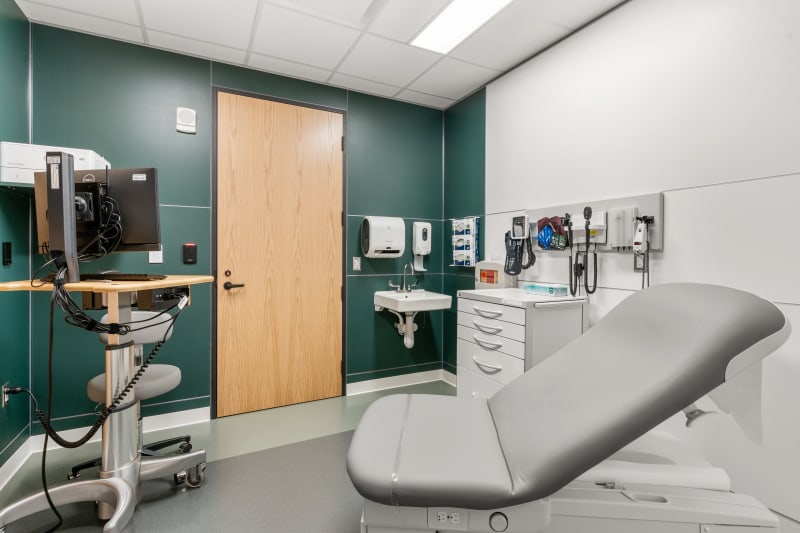
Or perhaps a subcontractor highlights, “these materials are more available in my region, and they have a better price range than this other one. So if you can look at this and consider your interior finishes, we think this will be better for us.”
But in order to share insights like these and be part of a problem solving equation, they need to be included in even the earliest planning conversations.
Updating the design process isn’t simple to execute, Guimaraes cautions. From rethinking approaches to contracts and adopting alternative methods of building — such as modular construction — to aligning capital and operational budgets, there are several factors to consider, she says.
Fortunately, the benefits of an evolved design process extend far beyond addressing today’s labor and supply chain challenges, “because we can design more for the team that is going to be building [the facility],” says Guimaraes. And ultimately build better healthcare spaces for patients.

Start by building collaboration into contracts
Design is in the details, including the paperwork. “One of the biggest challenges [to change] is how contracts are done,” Guimaraes explains. A litigious industry makes all parties wary of liability, errors, and omissions, she adds, which leads to an attitude that favors the status quo.
But collaborative contracts that acknowledge shared responsibility leave more room for innovation.
“We need to take a risk together … and if contracts are not written to allow that risk to happen, nobody is going to be willing to go all the way.”
It’s like dipping one toe in the ocean, instead of going for a swim — Guimaraes uses this analogy for unrealized potential. The full benefits of an evolved design process, from lower costs to faster delivery, can’t happen without everyone’s buy-in.
Modular design offers benefits that extend beyond speed to market
Another way to enhance efficiency in an updated design process is by adopting alternative methods — like off-site construction of modular interiors — that not only support speed to market, but better prepare healthcare facilities for future adaptation, says Guimaraes.

“If you look at the images of MRIs from the ‘70s and today, it’s hugely different. You look at images of an OR [operating room] from the ‘70s and today, you look at the size of a patient room from the ‘70s and today … there has been so much transformation.”
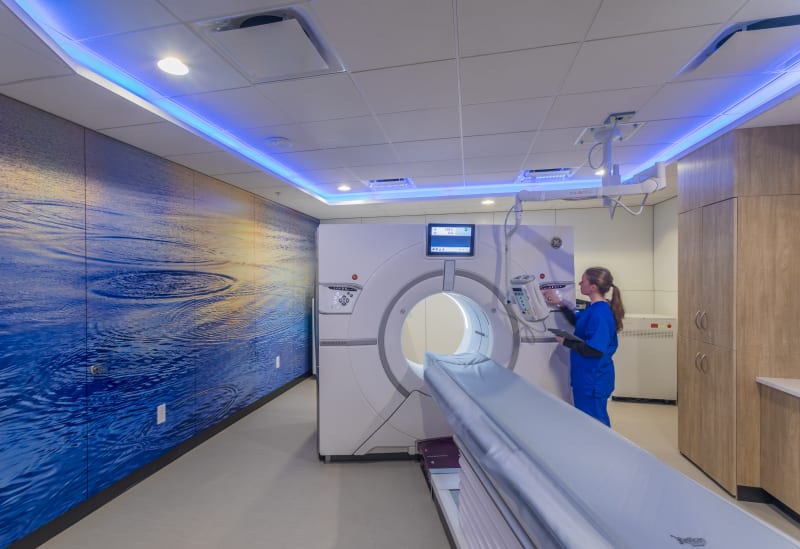
So how can healthcare spaces adapt to what might be required in the future?
Build modular spaces that make it easy to update a facility, even when more complex remodeling is required, says Guimaraes.
“It’s not so much that I’m expecting that I’m going to just push this modular wall out five feet and that is going to solve my problem. I’m going to have to remodel this space for whatever the need [then] is,” she explains. “I know there’s some level of investment in making a remodel. But do I have the capacity? Did I build the infrastructure right?”
Modular solutions can help meet these unknown future capacity needs.

But investment in modular can be hindered by the fact that “most institutions, they have capital and have operational costs, and they’re completely separate,” Guimaraes says.
Long-term savings associated with more adaptable infrastructure come from easier, quicker renovations, which then also reduces construction downtime. But operational savings can be hard to argue to a team managing a separate capital budget — who lean towards a more conventional design and construction process.
Again, expanded collaboration between these two silos can benefit the design process, the longevity of the spaces, and ultimately patient experiences, Guimaraes says.
“If you can come together and have [design and budget] conversations at all different levels … it’s really all for the staff, the patients, the caregivers, the families that are going to be going there.”
